Content
What is a stroke?
Complications after a stroke
- Paralysis
- Coma
- Brain swelling
- Aphasia
- Loss of coordination
- Apraxia of walking
- Relapse of the disease - why does it happen?
Who can have a stroke? Predisposing factors
- The main distinguishing features of female attacks
- In men
Precursors of stroke
The main thing is to see a doctor in time
Drugs for stroke
Caring for patients with dizziness after stroke
An important component of the rehabilitation treatment of patients with dizziness after a stroke is the organization of care and nursing. Impaired coordination of movements with preserved muscle strength in the limbs causes loss of self-care ability and a decrease in the functional activity of patients. They can cause injury and recurrent stroke.
In order to improve the quality of life of patients with dizziness, the latest technologies used in care are being introduced. Proper care is not opposed to treatment, but is organically included in it as an integral part and involves the creation of a favorable everyday and psychological environment at all stages of treatment. Due to the decrease in functional activity of patients with dizziness, he is recommended to use absorbent products (diapers for sedentary patients and absorbent panties for patients who have retained mobility).
After determining the cause of dizziness, an individual treatment regimen will be selected for you to get rid of the unpleasant consequences of a stroke. The use of modern recovery techniques allows specialists at the Yusupov Hospital Rehabilitation Clinic to improve the quality of life of patients suffering from dizziness after a stroke. Make an appointment with a neurologist by phone in advance.
What is a stroke?
The disease is an acute circulatory disorder in the human brain. The attack develops rapidly. It takes from a few minutes to several hours for a person to be seriously injured - sometimes irreversibly. Doctors call the limit of providing effective assistance a time period of 6 hours. After this, the patient will no longer be able to recover if he survives. The consequences of a stroke are the death of brain cells due to oxygen starvation.
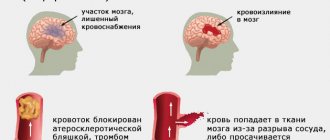
The two most common types of stroke are:
- By ischemic type (ischemic) – occupies a share of 75%. The peculiarity of this pathology is blockage of blood vessels or their compression. Damage occurs as a result of the presence of embolism, thrombosis and some other pathologies of the blood, blood vessels, and heart. Mortality rate is up to 15%.
- By hemorrhagic type (hemorrhagic) - occurs in 20-25% of cases. In this type of stroke, blood vessels rupture and bleeding occurs in the brain. Mortality rate – up to 35%.
Very rarely (up to 7% of cases) subarachnoid hemorrhage occurs. Its causes are traumatic brain injury or rupture of an arterial aneurysm (also due to trauma to the patient). In this case, the hemorrhage is directed into the space between the soft and arachnoid membranes of the brain. As a result of such a “blow”, more than half of the victims die.
You can undergo an examination in our clinic at the address: St. Petersburg, st. Bolshaya Raznochinnaya, 27 metro station Chkalovskaya
Correction of dizziness in patients with cerebral ischemia
Difficulties in implementing methods for effective correction of the main clinical manifestations of acute (especially chronic) forms of cerebrovascular pathology in our country are associated with the above-mentioned medical and social problems, as well as the lack of objective epidemiological data on the incidence of various forms of cerebrovascular pathology. If to date, thanks to the efforts of the National Association to Combat Stroke, many regions of our country have statistics on acute strokes [Skvortsova V.I., Gusev E.I., Stakhovskaya L.V., 2003, 2007], then real data on There are practically no patients with chronic cerebral ischemia. These patients are most often observed and treated in primary outpatient clinics, where the lack of qualified neurologists often leads to errors in diagnosis. A trip to the clinic for patients in this group is often physically and psychologically difficult; sometimes they are observed only by a local therapist and they are given “complex” diagnoses, where cerebrovascular pathology, especially in the early stages, is not taken into account at all, and in later stages is not always classified even among the complications of systemic atherosclerosis and arterial hypertension. The standard diagnosis of “coronary heart disease” for local therapists and general practitioners is “familiar”, familiar and often made without much thought, and to make a diagnosis of “chronic cerebral ischemia”, despite the clear clinical picture, a consultation with a neurologist is also required (preliminary record for 2-3-4 weeks), and the results of repeated examinations. The prescription of effective therapy to correct the steadily developing clinical manifestations of the disease is put on the back burner. It should be noted that many manifestations of cerebrovascular disease form clinical syndromes quite early, which lead to social and everyday disadaptation. It is the syndromes of clinical and everyday maladjustment that intensify both subjective complaints and the objective severity of the disease, closing a vicious circle of deterioration in the patient’s quality of life, from which he often cannot find a way out either on his own or with the help of a doctor. Dizziness of varying severity is often an integral clinical component of both acute cerebrovascular insufficiency (primarily acute stroke, including vertebrobasilar localization) and various forms of chronic cerebral ischemia. Chronic cerebral ischemia (CHI) is a special form of vascular cerebral pathology, considered as a slowly progressive diffuse functional and morphological damage to the brain substance, resulting from a decrease in cerebral blood flow as a result of the involvement of cerebral vessels in the pathological process. There are several forms of chronic cerebrovascular diseases: subcortical arteriosclerotic encephalopathy; multi-infarction condition; chronic cerebral vascular insufficiency due to pathology of the main arteries of the head; mixed forms (the most common combinations of subcortical arteriosclerotic encephalopathy and a multi-infarction state, a multi-infarction state and chronic cerebrovascular insufficiency) [Vereshchagin N.V., Morgunov V.A., Gulevskaya T.S., 1997; Yakhno N.N., et al., 2006; Skoromets A.O. 2005, 2006; Kalashnikova L.A., Gulevskaya T.S. 1998; Kotov S.V., 2001]. The varying severity of the clinical manifestations of chronic ischemia makes it possible, quite roughly, for the convenience of clinical practice, to distinguish several stages of the disease. Thus, the compensation stage is characterized by such subjective disorders as frequent headaches, irritability, decreased attention, moderate impairment of working memory and performance, sleep disturbance, absent-mindedness, general weakness with high fatigue, changes in life values, emotional lability, instability when walking; Episodes of dizziness of a non-systemic nature are typical, and initial symptoms of depression are often detected. If at this stage long-term adequate symptomatic and pathogenetic therapy is started, then it is possible to eliminate the symptoms. In the subcompensation stage, patients present similar complaints, however, attention is drawn to an increase in fatigue and a progressive decline in cognitive functions (attention and memory), an increase in intellectual and emotional disorders (neurotic and depressive reactions), a significant decrease in performance, more frequent and intense dizziness, significantly reducing quality of life of patients. It is at this stage that the patient’s maladjustment syndromes in the surrounding society begin to be clearly visible. In the stage of decompensation, the volume of complaints usually sharply decreases, which is due to a decrease in patients’ criticism of their condition. Along with this, there are clear complaints of memory loss, noise and heaviness in the head, sleep disturbances, instability when walking, severe persistent dizziness, usually occurring against the background of an increase or decrease in blood pressure, often occurring as vertebrobasilar vascular crises. The severity of intellectual-mnestic and focal neurological disorders increases. Upon examination, patients reveal persistent clinical signs of two or more neurological syndromes: pyramidal, discoordination, pseudobulbar, amyostatic, psychoorganic. Such patients are usually unable to work, since their social and everyday adaptation is severely impaired; they often require constant outside care, differing from patients with acute stroke only in the rate at which symptoms arise. In the pathogenesis of both acute and chronic cerebral ischemia in patients with CVD, systemic and local factors are important, leading to the emergence and progression of dysregulation in the functioning of the “blood flow-metabolism” system. The most unfavorable effect is exerted by the combined influence of several factors that determine the severe and rapidly progressing course of the disease. Systemic factors include, first of all, disturbances of systemic hemodynamics that arise as a result of a decrease in the pumping function of the myocardium, an increase or decrease in systemic blood pressure; disruption of autoregulation of cerebral blood flow. A significant contribution to systemic disorders that provoke the progression of cerebral ischemia is made by the pathology of hemostasis: the appearance of spheroid and folded forms of erythrocytes and their conglomerates; change in their deformability; increased aggregation of formed elements and blood viscosity; change in endothelial cell volume; violation of coagulation potential; imbalance of components of the blood coagulation and anticoagulation systems, etc. Local factors causing the progression of ischemic cerebral disorders include atherosclerotic stenosis and occlusion of intra- and extracranial vessels that perform transport (main arteries of the head) and distribution (arteries located on the surface of the brain) functions. The role of “steal” syndromes and cerebral hypoperfusion, including those caused by taking antihypertensive drugs, vasodilators and reoprotectors, needs additional study [Odinak M.M., Voznyuk I.A., 2007]. A local factor provoking cerebral ischemia with a clinical picture of dizziness syndromes is often spinal pathology, including: dorsopathy caused by osteochondrosis and spondylosis with compression of the vertebral arteries; whiplash; additional cervical ribs; Iatrogenic influences, including unprofessional use of manual therapy methods. Cerebral hypoperfusion, which occurs when the vascular systems are damaged at the macro- and microcirculatory levels, stimulates excessive synthesis of nitric oxide, which leads to additional disruption of vasoconstrictor-dilator mechanisms, autoimmune shifts and the formation of persistent local extra- and intravascular inflammatory reactions that support long-term persistence of clinical symptoms, as shown in Figure 1. With the predominant involvement of vertebral vessels in the pathological process, the mechanisms described above form a persistent picture of vertebrobasilar insufficiency, manifested primarily by dizziness, which becomes a syndrome that sharply reduces the quality of life of patients. Dizziness occurs in almost 15% of patients with various types of neurological pathologies, and during a therapeutic appointment it occurs in 24% of patients [W. Osterveld, 1991]. What is “dizziness?” Dizziness is the illusion of movement in a stationary environment, as well as the sensation of rotation or movement of one’s body as a result of a mismatch of information between its sensory systems. By dizziness, patients themselves often understand a variety of sensations: rotation; falls; moving your body or surrounding objects; lightheadedness, anxiety; severe general weakness; premonitions of loss of consciousness; unsteadiness when walking; impaired coordination and gait. Dizziness of almost any origin may be based on morphological causes (ENT pathology, tumors) or a mediator imbalance of a vascular, atrophic, metabolic nature, caused by peripheral or central vestibular disorders, multiple sensory deficits, psychogenic disorders, circulatory disorders in the brain stem, cardiovascular diseases . Why is dizziness syndrome caused by so many different causes? And why is dizziness such a common clinical symptom in acute or chronic vascular pathology of the brain? This is due to the fact that the normal activity of brain structures is ensured by the coordinated activity of sensory systems of equal importance, disturbances in the functioning of which lead to dizziness, as shown in Figures 2 and 3. In conditions of vascular pathology of the brain, dizziness is associated both with pathology of the vertebral artery, which provides blood supply to the inner ear and the functioning of vestibular mediator systems, depending on the balance of the neurotransmitter histamine, and with the frequent loss of regulatory central cerebral influences. This combination is the most common cause of dizziness in people with vascular risk factors. Vascular dizziness usually begins acutely, lasts several minutes, and is accompanied by imbalance, nausea and vomiting. The cardinal sign of vertebrobasilar insufficiency are additional symptoms: blurred vision, double vision, dysarthria, falls, weakness and numbness in the limbs. Is there a safe remedy for effective symptomatic treatment of dizziness? Since very often a patient with dizziness needs help immediately, he is ready to receive this help from the hands of any specialist: a general practitioner, ambulance, local therapist, neurologist, etc. It has already been noted that the adequate functioning of the vestibular mediator systems depends on the level of the neurotransmitter histamine. Histamine has a pronounced local vasodilator effect and actively interacts with specific receptors, providing adequate local stimulation; energy conversion; control of behavior, neuroendocrine and some autonomic functions. For the first time, histamine was used as a therapeutic agent by the American otologist D. Shambaugh (1980), who tested it on himself for the treatment of Meniere's disease. The drug Betaserc (betahistine) is a pharmacological analogue of histamine, effective when taken orally for the treatment of dizziness, including vascular origin. The wide range of pharmacological activity of the drug is due to its complex action at three levels: on the cochlear blood flow, on the central and peripheral vestibular apparatus. Due to this multicomponent action, Betaserc inhibits the pathological activity of the vestibular nuclei, causes vasodilation in the inner ear and stimulates blood flow in the vertebrobasilar system, actively relieving the clinical manifestations of vertigo syndrome, including in patients with symptoms of acute and chronic ischemia in the vertebrobasilar vascular system system. Today, Betaserc is a safe medicine with proven effectiveness in treating the symptoms of dizziness and can be used as a first aid remedy even before the exact genesis of the disease is established. The standard dosage of the drug is 24 mg 2 times a day. The presence of this drug in the patient’s personal medicine cabinet allows for both treatment and prevention of more severe symptoms of dizziness. It should be noted that fairly rapid relief of the clinical symptoms of dizziness, usually following the administration of adequate doses of the drug, does not subsequently relieve the physician of responsibility for conducting a complete clinical and instrumental examination of the patient with symptoms of dizziness, which should include an assessment of complaints and medical history, a detailed general examination, examination of the neurological status, the earliest possible CT/MRI to exclude a space-occupying lesion, ultrasound examination of the main arteries of the neck and head, radiography of the cervical spine, examination of hearing, the vestibular sphere, consultation with an otoneurologist. When establishing or confirming a diagnosis of vascular pathology of the brain, the attending physician is obliged, in addition to symptomatic therapy, to carry out long-term punctuated complex syndromic therapy, including: correction of blood pressure to levels that ensure adequate cerebral perfusion, oxidative stress, which causes progression of damage to neuronal formations, as well as disturbances in the rheological properties of blood and neurotransmitter disorders.
Literature 1. Aronov D.M., Zaitsev V.P. Methodology for assessing the quality of life of patients with cardiovascular diseases.//J. Cardiology.–2002.–No. 5–pp.92–95. 2. Belova A. N. scales, tests and questionnaires in neurology and neurosurgeons // guide for doctors. 2004, Moscow, Medical book, 456 p. 3. Boyko A.N., Sidorenko T.V., Kabanov A.A. Chronic cerebral ischemia (dyscirculatory encephalopathy) // J. Consilium medicum. 2004, vol. 6 No. 8, pp. 598–601. 4. Varakin Yu.Ya., Gornostaeva G.V. Prevalence of various forms of cerebrovascular pathology in the working age population. // Appendix to the journal. neurology and psychiatry named after. S.S. Korsakov issue 9. – 2003. – p.112. 5. Varakin Yu.Ya., Vereshchagin N.V., Arabidze G.G., Suslina Z.A. Arterial hypertension and stroke prevention: A brief guide for doctors. – M., 1996. 6. Vereshchagin N.V., Morgunov V.A., Gulevskaya T.S. Pathology of the brain in atherosclerosis and arterial hypertension. – M. Medicine, 1997. – 287 p. 7. Vladimirov Yu.A. Free radicals and antioxidants.//Bulletin of the Russian Academy of Medical Sciences. 1998. No. 7. P.43–51. 8. Gusev E.I. The problem of stroke in Russia.// supplement to the journal. neurology and psychiatry named after. S.S. Korsakov issue 9. – 2003. – pp. 3–5. 9. Gusev E.I., Skvortsova V.I. Brain ischemia. – M., 2001. 400 10. Damulin I.V. Alzheimer's disease and vascular dementia / ed. N.N. Yakhno. M., 2002. P. 85. 11. Damulin I.V., Parfenov V.A., Skoromets A.A., Yakhno N.N. Circulatory disorders in the brain and spinal cord // Diseases of the nervous system. Guide for doctors / ed. N.N. Yakhno, D.R. Shtulman. M., 2003. pp. 231–302. 12. Damulin I.V., Bryzzhakhina VG, Yakhno NI. Disturbances in walking and balance in dyscirculatory encephalopathy. Clinical, neuropsychological and MRI comparison. Neurol. judge 2004; 4:13–8. 13. Shmidt E.V. Vascular diseases of the nervous system. Ed. M: Medicine, 1975– 14. Zozulya Yu.A., Baraboy V.A., Sutkova D.A. Free radical oxidation and antioxidant protection in brain pathology /, M. “Znanie-M”, 2000, – 226 p. 15. Kadykov A.S., Shakhparonova N.V. Treatment and prevention of vascular diseases of the brain.// J. Consilium medicum. 2005, v. 7 No. 2, pp. 147–153 16. Kalashnikova L.A. Cognitive impairment and dementia in cerebrovascular diseases.// journal. Atmosphere. Nervous diseases. No. 2. – 2005. – pp. 36–40. 17. Kalashnikova L.A., Gulevskaya T.S., Kadykov A.S., Shakhparonova N.V. Subcortical arteriosclerotic encephalopathy (clinical and morphological study) // Nevrol. magazine. – 1998. – No. 2. – P. 7–12. 18. Karpov R.S., Dudko V.A. Atherosclerosis: pathogenesis, clinical picture, functional diagnosis and treatment. //Tomsk. 1998. 665 p. 19. Kotov S.V., Isakova E.V., Ryabtseva A.A., Lobov M.A., Rudakova I.G. Complex therapy of chronic cerebral ischemia / Ed. V.Ya. Neretina. – M., 2001. – P.5–32 20. Levin O.S., GolubevaLV. Heterogeneity of moderate cognitive disorder: diagnostic and therapeutic aspects. Consilium. 2006; 12: 106–10. 26 21. Levin O.S., Sagova M.M., Golubeva L.V. Factors influencing the life factors of patients with dyscirculatory encephalopathy with moderate cognitive disorder. Ross. honey. magazine 2006; 2: 22. Martynov A.I., Shmyrev V.I., Ostroumova O.D. et al. Features of damage to the white matter of the brain in elderly patients with arterial hypertension // Clinical Medicine. 2000. No. 6. pp. 11–15. 23. Novik A.A., Ionova T.I. Study of quality of life in medicine / Ed. Yu.L. Shevchenko. - M.: Geotar-Med, 2004. - P. 12-13. 24. Romanenko I. A. experience in assessing the level of “quality of life” in patients with chronic cerebral ischemia//advances of modern natural science.–2006. No. 8 pp. 36–37. 25. Rumyantseva S.A. Intensive therapy of ischemic stroke. RMJ, 2005, No. 2, pp. 1256–1259 26. Skoromets A.A., Melnikova E.V., Golikova R.V. Rational approach to vascular therapy of chronic cerebrovascular insufficiency.// journal. Atmosphere. Nervous diseases. No. 1. – 2005. – pp. 29–31. 27. Suslina Z.A., Varakin Yu.Ya. Arterial hypertension and prevention of cerebrovascular diseases. Position of a neurologist.//journal. Atmosphere. Nervous diseases. No. 4. – 2004. – pp. 2–8. 28. Yakhno N.N., Lokshina A.B., Zakharov V.V. Mild and moderate cognitive impairment in dyscirculatory encephalopathy // Clinical gerontology. 2005. T. 11. No. 9. P. 38–39. 85–92. 29. Yakhno NL., Damulin IV., Zakharov VV. Discircular encephalopathy. M., 2000. 30. Yakhno N., Levin O.S., Damulin I.V. Comparison of clinical and MRI data in dyscirculatory encephalopathy. Cognitive impairment. Neurol. magazine 2001; 3:10–8. 31. YakhnoNV, Damulin IV Advances in neurogeriatrics. Edited by M MMA, 1995; 189–228. 32. Bogousslavsky J. The global stroke initiative, setting the context with the International Stroke Society // J Neurol Sciences. 2005. V. 238. Supp l.1. IS. 166. 33. Bowler JV, Hacbinski V. The concept of vascular cognitive impairment. In T. Erkinjuntti, S. Gau–thier (eds). Vascular cognitive impairment. Martin Dunitz 2002; p. 9–26. 34. Court JA, Perry EK, Kalaria RN. Neurotransmitter changes in vascular dementia]. O'Brien et al (eds). Cerebrovascular disease, cognitive impairment and dementia. London. Martin Dunitz, 2004; 133–52. 35. Daneshnar B., Frandsen H., Autrup H. // Biomarkers. —1997. —V. 11, No. 2. -R. 117-123. 36. Fragata M. Model of singlet oxygen scavenging by a-tocoferol in biomembranes. //Chem. and Ph. Lipids. 1990. V. 27. No. 2. P. 93–99.
Complications after a stroke
Paralysis
This complication occurs when the motor center is involved in the pathological process. Most often, hemorrhage occurs in the left hemisphere of the brain, as a result of which the right side of the body is “taken away”. Paralysis can also be left-sided. As a result, the patient cannot contract muscles or make any movements. At the same time, behavior and perception of the surrounding world differ in patients with right- or left-sided paralysis. Often there is a mental disorder (excessive aggression, for example) or thinking.
Coma
This condition can last from several hours to several years. Coma occurs due to damage to the cortex and subcortical substance of the brain, as a result of which all signals are inhibited. In a coma, the patient's breathing and cardiac function are depressed, he is unconscious, and his reflexes are impaired. Some fall into a coma quickly, while others gradually. In the second case, within a few hours:
- the patient yawns frequently;
- general fatigue and malaise are felt;
- pulse changes;
- the body goes numb;
- coordination of movements is impaired;
- limbs lose sensitivity and mobility;
- there is a disturbance of consciousness;
- breathing activity becomes superficial.
Brain swelling
One of the most dangerous manifestations of a stroke. Symptoms include: convulsions coupled with psychomotor excitability, headache, nausea and vomiting against the background of increased intracranial pressure.
Edema is divided into two types:
- Cytotoxic. Brain cells swell due to a lack of oxygen and adenosine triphosphate. As a result, membrane pumps do not work properly, sodium ions penetrate into the cells, and water accumulates.
- Associated with impaired outflow of intercellular and interstitial fluids, as well as blood. Occurs when capillaries are damaged.
Aphasia
Impaired speech and writing ability. May include an inability to understand what others are saying, slow speech, and difficulty remembering and writing.
Loss of coordination
During a stroke, muscle tone and coordination of movements are impaired. As a result, a person cannot move without assistance. The muscles also spasm, as a result of which the patient’s actions are even more difficult, since he is forced to overcome the resistance of his own body.
Apraxia of walking
A person can take steps, but in general the process of walking cannot be controlled.
Relapse of the disease, why does it happen?
Provoking factors for the second and subsequent attacks are atherosclerosis, hypertension, thrombosis, abnormal vascular structure, and diabetes. In addition, patients often harm themselves. Having overcome the first difficulties, they neglect to visit the doctor and follow his recommendations. Many people return to bad habits and do not treat associated pathologies.
Causes of dizziness during stroke
Dizziness is divided into true, associated with damage to the vestibular analyzer, and non-systemic, which occurs outside the vestibular apparatus. In turn, vestibular vertigo is divided into three groups:
- peripheral (damage to the labyrinth);
- intermediate (occurs in the vestibular nerve);
- central (occurs in the central nervous system).
There are the following causes of central vertigo:
- acute ischemia in the brain stem (stroke, transient ischemic attack);
- chronic cerebral ischemia;
- whiplash injury to the cervical spine;
- brain injuries and tumors.
The most common causes of peripheral vertigo include Meniere's disease, vestibular migraine, and head injuries.
Dizziness during a stroke and after an acute cerebrovascular accident in 95% of patients is associated with damage or disruption of the blood supply to the cerebellum, which is responsible for a person’s balance and coordination in space. Disruption of the recovery process after a stroke (alcohol abuse, insufficient sleep, smoking) contributes to the persistence and recurrence of dizziness.
Poor nutrition, high levels of lipids, table salt, and simple carbohydrates in the diet slow down the process of recovery of brain cells. Physical and emotional stress, fear, and depression can cause dizziness as a result of autonomic dysfunction after a stroke.
A drop in blood pressure in stroke patients also causes dizziness and blurred vision. Diseases accompanying stroke (compression of the carotid arteries, osteochondrosis of the cervical spine) contribute to impaired blood supply to the brain and the occurrence of neurological symptoms.
Who can have a stroke? Predisposing factors
It is generally accepted that stroke occurs only in older people. However, in recent decades the disease has been rapidly becoming younger. An attack can occur as early as 40 years of age or even earlier.
Main risk factors:
- disturbances in sleep and nutrition when entering a “dangerous” age – over 50 years;
- hypertension;
- chronic heart disease;
- high stress loads at work;
- smoking and alcohol abuse;
- temporary, rapidly passing ischemic attacks;
- high blood cholesterol levels;
- obesity;
- diabetes mellitus (it increases the likelihood of not only the first, but also a second stroke);
- hereditary factor;
- lack of timely hospitalization during an attack and lack of qualified medical care in municipal hospitals;
- trauma (the rarest cause of stroke)
However, symptoms and causes differ between women and men.
The main distinguishing features of female attacks:
- the predominance of the disease is of the hemorrhagic type;
- very long and difficult recovery of functions;
- high mortality;
- high loads on blood vessels during pregnancy;
- Among the main causes are migraines, headaches, and great stress;
- it’s easier to see the first symptoms of an approaching “blow”;
- One of the provoking factors is taking oral contraceptives.
The most pronounced symptoms in women include: weakness, slowness of movement, shortness of breath, wheezing, increased heart rate, blurred vision, double vision, fainting, impaired hearing, pain on one side of the face and body, and unbearable headache.
In men
The main risk factors are impaired blood circulation, blockage of blood vessels, rupture of arteries with subsequent hemorrhage, blood thickening due to various diseases, obesity, diabetes mellitus, lack of physical activity, poor diet and eating disorders, bad habits, severe physical activity, vegetative-vascular dystonia, hypertension .
The main signs of a stroke in men may appear periodically, but go away over time. In this situation, the most dangerous thing is to decide that the trouble is over. After all, most likely, these are just transient ischemic attacks, signaling the approach of a stroke.
With the ischemic type, a man may feel dizziness, severe headache (it cannot be relieved by painkillers), weakness, decreased sensitivity in the limbs and numbness, short-term fainting, and vomiting.
A hemorrhagic attack is expressed by loss of consciousness, a sharp increase in pressure, the face becomes very red, noises are heard when breathing, facial asymmetry is noticeable, and vomiting occurs.
Dizziness during stroke. Treatment
To treat dizziness, doctors at the Yusupov Hospital take measures to eliminate the cause that caused it. This is of particular importance when dizziness occurs during cerebral stroke, which develops as a result of arterial hypertension, cerebral atherosclerosis, and diabetes mellitus.
For dizziness in patients with arterial hypertension, the underlying disease is treated. For this purpose, cardiologists individually select drugs for antihypertensive therapy. With the development of cerebral stroke, dizziness is caused by a transient or persistent disruption of the blood supply to the peripheral or central parts of the vestibular system. Most often it occurs as a result of ischemia of the vestibular nuclei of the brain stem. During a stroke, dizziness is accompanied by the following neurological symptoms:
- ataxia (impaired coordination of movements of various muscles in the absence of muscle weakness);
- oculomotor disorders;
- bulbar disorders (with damage to the glossopharyngeal, vagus and hypoglossal nerves);
- paresis (partial impairment of motor function) and paralysis;
- sensory disorders.
Dizziness increases the possibility of falls, injury to patients, limits their functional activity, and reduces the quality of life. In this regard, vestibular rehabilitation, stability training, and improvement of postural control are important tasks in the rehabilitation treatment of patients with stroke.
Comprehensive rehabilitation treatment for dizziness during stroke, which is carried out at the Yusupov Hospital, includes:
- pharmacotherapy;
- vestibular and oculomotor gymnastics;
- use of exercise therapy methods (biomechanotherapy);
- stabilization training with biofeedback effect.
In order to reduce dizziness in patients with stroke, doctors at the Yusupov Hospital use drugs from the following groups:
- neuroprotectors, which include inhibitors and antagonists. They help improve cerebral circulation and also protect the brain from repeated damage;
- Betaserc, a drug that helps cope with disorders, has proven itself well, regardless of the duration of dizziness;
- dizziness decreases with regular use of anticoagulants.
After stopping an acute attack of dizziness, rehabilitation specialists gradually begin vestibular gymnastics. It is a type of therapeutic exercises aimed at accelerating the adaptation of the vestibular system to damage caused by acute cerebral ischemia. When carrying out this method of rehabilitation treatment, the ability of various parts of the central nervous system to reorganize due to structural and functional changes is used. The patient is asked to perform a series of exercises that have a mild irritating effect on the vestibular structures. Repeatedly performing them leads to the patient getting used to the irritation and the dizziness subsiding.
To treat patients with dizziness after a stroke, biofeedback specialists at the Yusupov Hospital include stabilometric training in a comprehensive rehabilitation program. The technique is based on biofeedback, in which specialists use the parameters of the projection of the general center of mass onto the plane of support as a feedback signal. During special computer “stabilometric games”, patients learn to voluntarily move the center of pressure with varying amplitudes, speeds, degrees of accuracy and direction of movements without losing balance.
Precursors of stroke
Symptoms before an attack appear within a few days. However, many do not pay attention to them, because the signs of an impending stroke disappear on their own.
How to recognize the proximity of a “blow”? The most important harbingers:
- headaches that appear suddenly and go away quickly;
- weakness unexpected for a person;
- causeless nausea;
- short-term dizziness;
- frequent mood changes.
You also need to pay attention to symptoms such as:
- visual and hearing impairments;
- slow pulse;
- numbness of the limb;
- flushes of blood to the face;
- disturbance of speech function or coordination of movements;
- severe sweating.
If you have these symptoms, you should immediately consult a doctor, as it is still possible to prevent a stroke.
Within 3 hours from the moment of formation of a brain lesion, acute manifestations of a close “impact” occur:
- difficulty swallowing;
- unbearable headache that leads to fainting;
- severe dizziness;
- vomit;
- convulsions;
- breathing problems;
- tachycardia.
At this stage, the victim requires urgent hospitalization. With timely provision of first aid, the likelihood of severe complications will be reduced.
The main thing is to see a doctor in time
The doctor who treats strokes is a neurologist. He takes part in the restoration of lost mental and physical functions. The main tasks of a specialist when working with patients who have already been discharged from the hospital are secondary prevention, which is aimed at preventing a recurrent attack, as well as drug treatment of the consequences of the “stroke”.
A modern method for diagnosing pathology is ultrasound duplex scanning of neck vessels. An image of the vessel is formed, its patency and structure are displayed. Diagnostics allows timely detection and prevention of vascular diseases, including stroke.
You need to undergo the study if:
- frequent fainting, headaches, dizziness;
- hypertension;
- arrhythmias;
- elevated cholesterol levels;
- traumatic brain injuries;
- sleep, vision and hearing disorders;
- weakened attention, memory loss.
The necessary studies are prescribed by a neurologist. Based on diagnostic data, treatment is prescribed, which varies depending on the type of stroke.
Our clinic address: St. Petersburg, st. Bolshaya Raznochinnaya, 27 metro station Chkalovskaya
Diagnosis and treatment of noise in the head
When this unpleasant symptom appears, you should not waste time doing self-diagnosis, try to cope with it yourself, or hope that “it will pass.” The correct decision for the patient is to seek help from a specialist.
Diagnosis of diseases accompanied by noise in the head is carried out by doctors of various profiles - therapists, otolaryngologists, neurologists, psychotherapists/psychiatrists. But most often, patients with such a problem turn first to a neurologist.
First of all, the doctor’s task is to specify the noise, to understand what exactly the patient feels - a high-frequency squeak, ringing, buzzing, buzzing or hum, one- or two-sided, accompanied by pulsation or not; clarify the intensity of sensations and the symptoms that could accompany them. If the patient does not tell him himself, the doctor will ask leading questions about whether there is hearing loss, congestion in the ears, headache (usually occipital) pain, a tendency to increase or decrease blood pressure, find out what somatic diseases the person seeking his appointment suffers from. Human. Based on these data, the specialist will suggest what type of tinnitus he is dealing with - objective or subjective. Then he will conduct an objective examination - examine the organ of hearing and perform a number of tests necessary to make a diagnosis.
Shpidonov Gennady Stanislavovich
Neurologist
Rostov State Medical University (neurology)
10 years of experience
At the end of this diagnostic stage, the neurologist will make a preliminary diagnosis (or several putative diagnoses) and prescribe further examination to clarify it, in particular:
- general blood and urine analysis;
- blood biochemistry (lipidogram, coagulogram, ferritin);
- duplex or triplex scanning of neck vessels;
- MRI of the brain or cervical spine;
- consultation with an ENT doctor.
The scope of examinations is determined individually, depending on the specific clinical situation.
If a somatic doctor has not established the cause of noise in the head, he will assume the psychogenic nature of this condition and recommend that the patient consult a psychiatrist or psychotherapist. The specialist will have a targeted conversation with the patient, find out what complaints he has, focusing on feelings of anxiety or fear, decreased mood, especially in the morning, sleep disturbances, severe weakness, palpitations, sudden fluctuations in blood pressure, and will clarify whether this condition is permanent or temporary, not Is it related to stress? If a patient is suspected of neurosis, psychosomatic disorder or depression, the doctor will conduct a series of tests to clarify the diagnosis.
Only after the diagnosis has been established is it recommended to begin treatment for noise in the ear and head.
Medicines for noise in the head and ears
Conservative therapy often helps to cope with this symptom. Depending on the manifestation of which disease the noise is, the patient may be prescribed medications from the following groups:
- antibacterial, anti-inflammatory drugs (for infectious and inflammatory diseases of the ear);
- vascular drugs (improve blood circulation, nutrition of brain cells, dilate blood vessels);
- nootropics (improves metabolic processes in the cells of the nervous system);
- B vitamins (improve trophism of nervous tissue);
- trimetazidine (nourishes the heart muscle);
- iron supplements (if the noise is based on iron deficiency anemia);
- betahistine (for noise due to increased pressure in the cochlear labyrinth);
- antidepressants, anti-anxiety drugs, antipsychotics (if the pathology is psychogenic);
- sedatives, hypnotics – if the patient complains, it is not the inability to sleep;
- medications containing caffeine (for a tendency to low blood pressure, severe weakness and other symptoms of asthenia).
If the cause of the disease is cerumen, the doctor will wash it out of the ear and the noise will disappear.
Surgery
With confirmed damage to the autonomic nervous system, non-vibratory tinnitus can be eliminated by surgical intervention in the area of the nerves of the tympanic cavity or cervical sympathetic nodes.
Surgery on damaged structures of the tympanic cavity or cochlea will help get rid of objective noise.
Other treatment methods
As auxiliary methods of therapy, the patient may be prescribed:
- wearing a hearing aid, electrical stimulation of the auditory nerve (with decreased hearing acuity);
- physical therapy;
- massage;
- physiotherapy;
- psychotherapy.